Introduction
Welcome to this multiple choice question (MCQ) activity. It is one of a series of activities designed to give you an opportunity to test your knowledge to help you to identify strengths and gaps, to provide you with answers and reference material for further review and over time give you the opportunity to reflect on your progress.
All Registrars, at all training levels, in GPTQ will be completing these. GPTQ will also review your answers compared to your peers and give you feedback.
In this activity the multiple choice questions are single best answer of five (5) options.
In addition there are two other rating questions for you to complete. They appear after you have chosen your answer to the MCQ.
Option weighting. The first series of questions asks you to weight each answer according to likelihood of being correct (in MCQs options are all possible but some are more likely/correct than others). You need to drag each option slider to identify your perception of the weighting for that option.
Question confidence rating. This rating relates to how confident you are about your answer to the question as a whole. You can click on the rating boxes or use the slider. Your confidence rating will be reviewed at the conclusion of the activity so you can reflect on how confident you were across each question and across the whole activity.
Instructions
In this MCQ activity there are 30 MCQs for you to work through. You can work through them sequentially or choose questions from the menu in any order.
After you complete the MCQ, option rating and question confidence rating you are required to press the submit button to record your answers. Once you press the Submit button you will not be able to change your answers. You will immediately receive the correct answer and feedback so that you can compare them with your own answer. There will also be references provided for further reading.
At the end of the activity there is a conclusion screen that summarises the topic of each MCQ, whether your answer was correct/incorrect, your confidence level and the references for each MCQ. You can also print this summary screen so that you can explore the references at a later date.
Ideally you should complete this activity in one sitting, however you can click 'Save and close' to save and re-open it if you need to complete it in stages.
This activity should take 60 minutes to complete, or longer depending on whether you also explore the reference material at the same time.
Question 1: June - Influenza
You are a GP in a large town and are reviewing your pathology results. You note results of a throat swab which is positive for Influenza B, but a strain not covered by the current vaccine. The swab was collected two days prior after an appointment with June, aged 62 years.
June had given a two-day history of feeling unwell with fevers, cough and general aches. She is generally well with no ongoing medical problems and no regular medications. She works in school administration, and has a son Mark with Down syndrome who lives with her.
You phone June and inform her of the result. She tells you she is still feeling quite unwell with fevers and has spent most of the past few days in bed, though is not significantly breathless.
She has a number of questions, including whether she needs any treatment and whether Mark is also at risk. She tells you that Mark had the flu vaccination this year, but she didn’t get around to having it herself.
In discussing treatment, what is the most appropriate advice to give June?
Select an answer
Individuals most at risk for complications from influenza infection include very young children, elderly, those with chronic illness or immunocompromised, and pregnant women.
Mark’s Down syndrome would make him vulnerable to poor outcomes if he were to contract influenza. Thus the general recommendation would be to start a neuraminidase inhibitor as soon as possible for high risk individuals exposed to influenza, ideally within 48 hours of exposure – either oseltamivir or zanimivir for 10 days. The need for prophylaxis is also important as the vaccine Mark received does not cover the strain June has been infected with.
June herself would not be in a group at higher risk for complications of influenza, and thus treatment with antivirals would not be routinely recommended for her.
In otherwise healthy adults who have a low risk of complications, treatment with a neuraminidase inhibitor reduces duration of influenza symptoms by less than 1 day on average, when treatment is started within 48 hours of symptom onset. Such limited benefit must be balanced against the potential adverse effects of the antivirals.
Vaccination is an important step in prevention of influenza, but does not cover all strains of the virus.
Influenza is generally most infectious in the first 3-5 days after onset of symptoms (in children it can be up to 7-10 days); thus June could still be infectious. June should be advised to isolate herself as much as possible and continue appropriate hygiene measures, until at least 24 hours after fevers have resolved.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 2: Research - EBM, NNT
You have researched two randomised controls on the impact of intensive insulin therapy and the rate of worsening retinopathy. They each show that several years of insulin reduced the proportion of worsening retinopathy to 13% from 38%.
In thinking about your own diabetic patients, what does this mean in terms of the number of patients needed to treat (NNT) to see an improvement?
The Number Needed to Treat (NNT) is calculated as 1/AAR
The absolute risk reduction is EER – CER
CER. The Control Event Rate is 38%
EER. The Experimental rate is 18%
18% - 38% = 25% Absolute risk reduction (AAR)
NNT = 1/25% = 4
So, four patients need to be treated with intensive insulin therapy for one to achieve a favourable outcome.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 3: Caroline - Basal cell carcinoma treatment
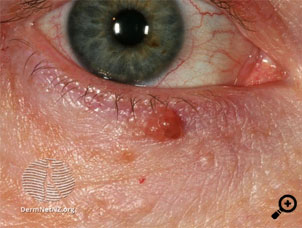
Caroline, aged 59 years, presents with a lesion on her right eyelid. It started about six months ago and she thought it might be a stye. However, it has slowly enlarged. It is not painful or itchy, and she is otherwise well.
The appearance of the lesion is shown in the picture.
What is the most appropriate treatment?
Select an answer
The provisional diagnosis is a nodular basal cell carcinoma (BCC). In this picture one can see the shiny, pearly nodule with a smooth surface and with linear telangiectasia apparent across the nodule.
Mohs micrographic surgery (a precise surgical procedure that involves carefully examining marked excised tissue under the microscope, layer by layer, to ensure complete excision) is most appropriate for BCCs that are:
- located where tissue conservation is required (e.g. nose, eyelid and around the eyes, centre of face).
- infiltrative (morphoeic or micronodular subtypes)
- poorly defined, so the extent of the tumour is not obvious clinically
Cryotherapy is suitable for small superficial BCCs on the trunk and limbs. It is best avoided for BCCs on the head and neck because the double thaw technique causes a sizeable blister and a hypo-pigmented scar.
Imiquimod is an appropriate treatment for a small superficial BCC, not a nodular BCC.
Incision and curettage is the appropriate treatment for a Meibomian cyst, which should not be confused with a nodular BCC.
Radiotherapy for BCCs is mainly used if surgery is not suitable, or it can be used after excision of an aggressive BCC. It is not recommended close to the eye. Radiotherapy can also be used in a squamous cell carcinoma when surgery is unsuitable – however this lesion is a BCC not an SCC.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 4: Brian - STEMI, fibrinolysis
You are working in a rural regional hospital emergency department. Brian, a 55-year-old Aboriginal man presents with severe central chest pain radiating to his left arm. The pain has been present for three hours.
The electrocardiogram (ECG) confirms ST elevation myocardial infarction (STEMI). The hospital doesn’t have access to percutaneous coronary intervention. Brian is given aspirin 300 mg orally, and you quickly arrange for fibrinolytic therapy. He does not have any contra-indications to fibrinolysis.
What is the most appropriate adjunctive therapy to be administered with the fibrinolysis?
Although either enoxaparin or unfractionated heparin are options for adjunctive therapy with fibrinolysis, the guidelines recommend enoxaparin over unfractionated heparin (NHF Guidelines 2018 p 920).
Unfractionated heparin is used with patients with severe kidney impairment or who have high risk of active bleeding that may require rapid reversal of anticoagulation (eTG).
Dual antiplatelet therapy when using fibrinolysis treatment is aspirin plus clopidogrel for a confirmed STEMI. Ticagrelor or prasugrel are not currently recommended because there is inadequate data on their safety and efficacy with fibrinolysis (eTG and NHF Guidelines 2016 p921).
Atenolol and enalapril are medications to be commenced and continued long-term for those with acute coronary syndrome following reperfusion.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 5: Simone - First episode psychosis management
Simone, aged 18 years, attends the general practice with her parents. They are concerned that she is “not her usual self”. She has stopped attending her local Technical and Further Education (TAFE) course for the past three weeks and is staying in her room for most of the time. She has also stopped wanting to see her friends.
Yesterday when her parents convinced her to go to the local coffee shop with them, she kept commenting that everyone “knew her” and could “read her mind”. Once she got home she closed all the blinds in the house and locked the all doors in the house.
Her parents think that she has hardly slept for the last three nights as they hear her pacing in her room and today she appears to be excessively anxious.
When you see Simone she seems dishevelled and very anxious. She doesn’t talk much but does reiterate that people can read her mind.
You are working in a rural area and can admit patients to the local hospital. You ring the psychiatrist and decide to admit Simone for investigation and treatment (with psychiatric support).
What is the most appropriate acute treatment of Simone?
The most likely diagnosis is a first episode psychosis, however other potential diagnoses need to be considered e.g. illicit substance abuse, bipolar disorder, major depression, schizoaffective disorder etc.
The guidelines suggest that no young person should be commenced on an antipsychotic during the first 24/48 hours of a first episode psychosis to allow for an anti-psychotic drug-free assessment phase. However short-term benzodiazepines can be successful for managing acute symptoms:
- agitation/aggression – e.g. diazepam
- anxiety e.g. lorazepam (choice for Simone because of her high level of anxiety)
- sleep disturbance e.g. temazepam
Risperidone is an appropriate second-generation antipsychotic, which may be prescribed once investigations have been undertaken and a diagnosis has been established. As most people with first episode psychosis respond to antipsychotics more quickly and to a greater extent than those with established disease, the aim is to ‘start low, and go slow’.
Escitalopram is used for the management of depression and lithium is an ideal mood stabiliser in bipolar disorder (however risperidone and other second-generation anti-psychotics (SGAs) can also be used for the treatment of acute mania or prevention).
Clozapine is reserved for treatment-resistant patients and other specific patient groups (e.g. persistent suicidal ideation, severe extrapyramidal side effects, marked aggressive behaviour).
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 6: Beth - Painless subacute thyroiditis
Beth, a 32-year-old woman, presents because she has noticed that her pulse is fast. She first became aware of it three weeks ago when she was doing a first aid course at work. Since then she has been checking it and it is still fast. She doesn’t notice any irregularity of the pulse. She has felt more lethargic and tired over the past two months, but she has no other specific symptoms.
Beth has no significant past medical history, is nulliparous, and her only medication is Implanon® (etonorgestrel implant).
Clinical examination is unremarkable apart from a regular pulse of 120/minute. An electrocardiogram (ECG) confirms sinus tachycardia.
Preliminary investigation results include:
- Thyroid stimulating hormone (TSH) - <0.01 mIU/L (normal range 0.5 – 4.0 mIU/L)
- Free thyroxine (T4) - 45 pmol/L (normal range 10-25 pmol/L)
- Free triiodothyronine (T3) –22 pmol/L (normal range 3.1 – 5.4 pmol/L)
A radionuclide thyroid scan shows near absent uptake.
What is the most appropriate treatment option for Beth?
The history and investigations indicate thyrotoxicosis, and the near absent thyroid uptake on radionuclide thyroid scan confirms the diagnosis of painless sporadic thyroiditis. Propranolol is the treatment of choice for managing hyperthyroid symptoms. In a young, otherwise well patient with mild or no symptoms, monitoring of thyroid function may be all that is required with no specific treatment needed.
Hyperthyroidism is usually present for 1-2 months and is often followed by hypothyroidism for 4-6 months. Thyroxine would be considered if the hypothyroid phase is symptomatic, prolonged or permanent (20%).
Carbimazole is first line treatment for Graves’ disease, and propylthiouracil is only indicated for maintenance therapy in the first trimester of pregnancy and/or when a patient has experienced adverse events with carbimazole. (eTG)
Subacute thyroiditis does not respond to either medication.
Radioactive iodine is the first-line treatment for thyrotoxicosis due to a toxic adenoma or toxic multinodular goitre.
The most common causes of hyperthyroidism are Graves’ disease, multinodular goitre, toxic adenoma, and subacute thyroiditis. Blood levels of T4, TSH and thyroid auto-antibodies along with ultrasound and/or radionuclide scan results will help to distinguish between different aetiologies.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 7: Robert - Hepatitis C specialist treatment
Robert, a 35-year-old man attends with a minor laceration to his left forearm. He tells you that he has a history of chronic hepatitis C, and you take appropriate precautions whilst suturing his wound.
You also take the opportunity to discuss with him the availability of oral therapies for the treatment of chronic Hepatitis C and that general practitioners can now be involved in prescribing treatment. However, you explain that there are still some patients who require referral directly to a specialist for their management. You review his history and investigations.
Which finding would indicate that Robert should be referred directly to a specialist for treatment?
Select an answer
Oral direct acting anti-virals (DAAs) have been available on the Pharmaceutical Benefits Schedule for the treatment of patients with hepatitis C virus (HCV) since March 2016. These medications can be prescribed by GPs in consultation with a hepatologist, a gastroenterologist or an infectious disease physician, allowing community-based treatment of most patients with uncomplicated chronic HCV.
There are guidelines published by the Gastroenterological Society of Australia which should be followed regarding the pre-treatment assessment of patients with chronic HCV.
A number of patient groups require specialist referral including:
- patients with cirrhosis (or a high likelihood of cirrhosis), including those with prior evidence of decompensated cirrhosis, such as encephalopathy, previous variceal bleeding or refractory ascites;
- those with significant comorbidities (e.g. chronic kidney disease with eGFR <50 mL/min/1.73 m2);
- those with concurrent infections (e.g. Hepatitis B Virus, Human Immunodeficiency Virus);
- those with relevant potential drug-drug interactions. (Khoo and Tse 2016)
Regarding the other response options:
- All HCV genotypes 1-6 are suitable for treatment with DAAs.
- HCV viral load (determined by polymerase chain reaction testing) must be determined to confirm current HCV infection before consideration of treatment. A negative test result means no need for HCV treatment.
- Patients who have failed to respond to previous “all-oral” / “interferon-free” treatment (sustained virologic response not achieved), should be managed by an appropriate specialist. (Strasser)
The treatment regimen and duration selected will depend on hepatitis C genotype, viral load, previous treatment experience and the presence or absence of cirrhosis.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 8: Kylie - Breast cancer risk factors
Kylie, a 54-year-old female, lives in a remote part of Queensland. As part of her consultation she asks the doctor about her risk factors for breast cancer.
The doctor asks a number of questions and discovers that Kylie had a high birth weight. She had two children, the first was born when she was 30 years old. She used the oral contraceptive pill until menopause. She has had two screening mammograms and she had moderate dense breast tissue identified. Her hobbies include regular cycling and she is a vegetarian.
Which factor, apart from her age, carries the greatest risk for breast cancer?
Select an answer
Of all the risk factors, age carries the greatest risk of developing breast cancer. Breast density is the second highest risk factor. Moderate breast density is associated with approximately a 1.53 increase, with extremely dense breasts associated with a 2.14 times risk compared to women with average breast density.
There is an increased risk of approximately 1.07 for every five years of oral contraceptive pill use, compared to those who have never used the pill. This risk gradually reduces after cessation with the risk after 10 years being similar to those who have never used the pill.
There is convincing evidence that older age at first birth (over 30 years of age) is associated with increased risk. This is estimated to be overall approximately 1.2.
Higher birth weight probably confers an increased risk for premenopausal breast cancer, but there is no conclusive evidence to suggest it is associated with an increased risk of postmenopausal breast cancer.
Living in an urban region compared to living in a rural or remote area is actually associated with a higher risk. The differences are thought to be due to a range of lifestyle and reproductive factors.
Protective factors mentioned in the history include large amounts of physical activity (0.83 for premenopausal and 0.90 for postmenopausal woman) and parity (0.93 reduction per birth). Being vegetarian (or eating a high amount of vegetables) may be associated with a decreased risk (evidence is only suggestive).
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 9: Kevin - Post herpetic neuralgia
Kevin, aged 75 years, presents complaining of right sided face pain. It has been present for over four weeks. Paracetamol was helpful for a while but the pain is worsening.
He describes sudden sharp stabbing pains that shoot through his right cheek. These can occur at any time, but even more often when he is showering or shaving.
His past history includes Type 2 diabetes, gout, hypercholesterolaemia and benign prostatic hypertrophy. His medications include metformin, atorvastatin and tamsulosin.
On examination you notice a few depigmented areas on his cheek and Kevin tells you that he had a mild rash on his face about the time the pain started. There are no other abnormal examination findings.
What is the most appropriate treatment option for Kevin?
The provisional diagnosis, with the history of a rash around the time of onset of pain, is post-herpetic neuralgia.
Of oral therapies the most effective evidence-based treatments for this condition, giving a response rate of around 40% - 65%, include:
- Tricyclic antidepressants – however these are not appropriate for Kevin given his benign prostatic hypertrophy and the possible anticholinergic effect of urinary retention from tricyclic anti-depressants
- Gabapentin
- Pregabalin
A topical 5% lignocaine patch is a suitable first line option (wear up to 12 hours) and has comparable efficacy to pregabalin.
Transcutaneous electrical nerve stimulation (TENS) is also often useful in conjunction with the adjuvant analgesics above; topical capsaicin could also be trialled. Psychological therapies are also recommended.
Tramadol or opioids are usually second line and used in conjunction with the adjuvant analgesics above.
Famciclovir is used acutely, within 72 hours of the onset of herpes zoster, to reduce the occurrence of post herpetic neuralgia.
Carbemazepine is used for the treatment of trigeminal neuralgia; it is not generally effective for post herpetic neuralgia.
Post herpetic neuralgia is a debilitating complication of acute herpes zoster, and occurs in up to 75% of patients over the age of 70 years after an episode of shingles. Trigeminal neuralgia can cause a similar history regarding pain distribution and characteristics, but would not be preceded by a rash.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 10: James - Haematuria, IGA nephropathy
James, an 18-year-old university student, presents to you concerned that he had pink discolouration of his urine this morning.
Upon further questioning, he tells you that his urine has always appeared yellow in colour until today, and he denies any abdominal pain, dysuria, urinary frequency, urethral discharge, or penile skin lesions. He reports having a sore throat and sniffles for a day or so, but says that he is otherwise well. He is sexually active.
A urine dipstick test shows 4+ red blood cells and 1+ protein.
On examination, James looks well. His vital signs are: Temperature 37.8°C; pulse 92/minute and regular; blood pressure 150/90 mmHg; respiratory rate 12 /minute. His ear, nose and throat examination shows a reddened pharynx with no other abnormalities. His cardiorespiratory, abdominal and genital examinations are normal. He has no rashes.
The most likely diagnosis is:
Select an answer
This presentation has the hallmarks of nephritic syndrome with “sub-nephrotic range proteinuria, hypertension and haematuria.” (N.B. Nephrotic range proteinuria is the loss of 3 grams or more of protein into the urine daily; it is usually apparent in 3+ and 4+ readings on a dipstick.)
IgA nephropathy is the commonest cause of glomerulonephritis/nephritic syndrome in Australia. It typically presents as haematuria in a young male adult at the time of, or within 1-2 days of a mucosal infection such as URTI, influenza or throat infection, and lasts for several days. It results in deposition of IgA antibody complexes in the glomeruli, and can run a variable course. Any suspected cases should be immediately referred for biopsy.
Chlamydia urethritis is unlikely because whilst it can be asymptomatic, common presenting symptoms are dysuria and penile discharge. Proteinuria and hypertension would be unusual. In young men, a history of dysuria is a sexually transmitted infection unless proven otherwise. (ASHA)
Non-specific urethritis is the term used to describe inflammation of the urethra (generally in men) when gonococcus or chlamydia is not the cause. In men, symptoms often include a watery penile discharge and dysuria; haematuria and hypertension would not generally be present. There is often no cause found on testing, but it has been postulated that bacteria such as Ureaplasma, viruses such as Herpes Simplex and parasites such as trichomonas can be causative.
Acute post-streptococcal glomerulonephritis (PSGN) occurs most commonly in children aged >5 years, especially in Indigenous communities, following Group A beta haemolytic streptococcal infection of throat or impetigo. The strep infection usually precedes renal symptoms by 1-2 weeks. This is in contrast to IgA nephropathy in which the renal symptoms occur at the same time as the strep infection or sore throat.
A urinary tract infection (UTI) needs to be considered but is less likely in this scenario. UTIs are very uncommon in young men. Dysuria is the most frequent symptom of UTIs in men, with the combination of dysuria, urinary frequency and urinary urgency being about 75% predictive for a UTI. Nearly all patients (≥ 96%) with UTI have pyuria (positive leucocyte esterase) on dipstick testing. Urine dipstick testing may also show nitrites, blood and protein.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 11: Trina - Treatment vestibular neuronitis
Trina, aged 58 years, presents with four hours of severe dizziness and nausea. When she woke up this morning and went to get up she was very dizzy and felt unsteady. Over the next three hours the dizziness has worsened and she “can’t walk straight”. She went back to bed and laid on her right side with her eyes closed to “stop the room spinning”. She denies any hearing loss or tinnitus. She has vomited once.
She has a past history of hypertension, hypercholesterolaemia, and irritable bowel syndrome for which she takes metoprolol, simvastatin and a high fibre diet.
On examination there is a torsional nystagmus with fast phase to the right on looking to the right or left. The nystagmus increases when looking to the right. There is no vertical skew. The head impulse test is positive. There are no other neurological findings.
Assuming the most likely diagnosis for this clinical presentation, what is the most appropriate treatment?
The findings in this patient - abnormal head impulse test, and unidirectional nystagmus and no vertical skew - suggest a peripheral cause for the vertigo. As there is no tinnitus or hearing loss the most likely diagnosis is vestibular neuronitis.
Current evidence indicates that prednisolone (1mg/kg up to 75mg) may hasten recovery from vestibular neuronitis, so it is worth offering this treatment option to patients. Prochlorperazine, promethazine and diazepam may be used for acute symptomatic management but should not be used long term.
The Epley manoeuvre is treatment for benign paroxysmal positional vertigo. The history would be one of pure motion-induced dizziness and vertigo that is short term lasting minutes not hours.
Hydochlorthiazide with or without betahistine is used in Meniere disease.
Sumatriptan may be effective for acute vestibular migraine.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 12: Sally - Migraine no aura and contraception
Sally, aged 35 years, presents because of recurrent headache. She is worried as she has had four episodes of headache over the last three months.
She describes them as throbbing headaches, which are always associated with nausea. On one occasion she vomited with the pain. The headaches always occur over her left temporal region. On specific questioning she has noticed that bright lights and loud noises bother her when the headache is present, but she denies any other symptoms. She has never had anything similar in the past.
She has been well in the past. Her only medication is Microgynon 30® (30mcg ethinyloestradiol and 150mcg levonorgestrel).
She doesn’t have the headache at present and her physical examination is unremarkable.
You explain your provisional diagnosis and management for the headaches to Sally.
In light of her headaches, what contraceptive option conveys the best safety profile?
Select an answer
Sally has a provisional diagnosis of recent onset of migraine without aura. The UK Medical Eligibility Criteria (UKMEC) identify the initiation of contraception with a copper IUD in someone with migraine without aura, at any age, as Category 1 (a condition for which there is no restriction for the use of the method).
These guidelines also advise that continuation of a combined hormone contraception (such as her current oral contraception Microgynon®, or a NuvaRing®) in a woman with new onset of migraine without aura, at any age, has a category 3 risk – i.e. it is a condition where the theoretical or proven risks usually outweigh the advantages of using the method. It is not recommended if there are other more appropriate methods available.
Progesterone-only contraception specifically Depo-progesterone and Implanon have a Category 2 rating – “advantages of using the method generally outweigh the theoretical or proven risks”. The progesterone only pill has a Category 1 rating for initiation with migraine with aura, but Category 2 for continuation. Progesterone-only contraception could be discussed with Sally along with the option of a copper IUD, with Sally considering the pros and cons in association with her preferences.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 13: Graham - Eye stye, hordeolum
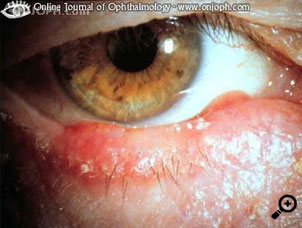
Graham, a 35-year-old man, presents with a painful lesion on the lower lid.
What is the most appropriate treatment?
Select an answer
This is a stye or external hordeolum, which is an abscess of the sebaceous gland associated with an eyelash. Frequent warm compresses will allow the stye to point and discharge spontaneously. Removal of the eyelash often aids resolution. There may be an underlying blepharitis present.
Topical antibiotics are not required. Oral anti-staphylococcal antibiotics are indicated if there is an accompanying cellulitis.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 14: Bob - Prostate cancer treatment side-effects
Bob, a fit and active 58-year-old, presents to discuss his options following a diagnosis of prostate cancer. The letter from the urologist indicates that he has clinical stage T2b cancer with a Gleason score of 8 and prostate specific antigen (PSA) test of 18ng/ml. He is offering Bob a radical prostatectomy.
Bob is concerned about possible complications after the procedure and wants to discuss these with you.
Which complication occurs most frequently following a radical prostatectomy?
Retrograde ejaculation occurs in all radical prostatectomies. The table below (from Duchesne 2011) outlines the approximate rates of complications
Complication |
Estimated risk |
Retrograde ejaculation |
All |
Erectile dysfunction |
30–100% |
Urinary incontinence – any |
Up to 70% |
Gastrointestinal effects |
Less than 15% |
Urethral stricture |
Up to 10% |
Urinary incontinence – severe |
0–5% |
Clear discussion of complications is important as the evidence indicates that most patients remember less than 50% of what was communicated.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 15: Julia - Anaphylaxis, iron infusion
Julia, aged 42 years, has been diagnosed with an iron deficiency anaemia due to menorrhagia.
Her ferritin is very low and you discuss the option of an intravenous (IV) infusion. You are able to organise this at your local regional hospital.
What factor in her history, would be most likely to increase the risk and/or severity of a hypersensitivity reaction from an iron infusion?
Select an answer
The following may worsen the outcome of a hypersensitivity reaction if it occurs:
- Medications – beta blockers and ACE inhibitors (e.g. enalapril)
- Severe respiratory or cardiac disease
- Old age
Anxiety (patient or staff) has also been suggested to increase the risk of hypersensitivity reactions.
There are a number of factors that increase both the incidence and severity of hypersensitivity reactions with IV infusions:
- Type of iron product used
- Previous reaction to IV iron
- Fast iron infusion rate
- History of other drug allergy or allergies
- Severe asthma or eczema
- Mastocytosis
There is equivocal evidence that the presence of systemic inflammatory diseases such as rheumatoid arthritis and systemic lupus erythematosis (SLE) increase the risk of hypersensitivity reactions, and there is some evidence that IV iron may be beneficial in these disease states.
Iron infusion is contraindicated in the first trimester of pregnancy.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 16: John - Diabetes cycle of care
Your practice manager is discussing how best to implement the Medicare Benefits Schedule Diabetes Cycle of Care with you. You are working through the files of a few of your patients with diabetes.
John was diagnosed with diabetes 12 months ago. His medical records show the following assessments and activities have been undertaken in the past 12 months:
- At diagnosis:
- HBA1c measured
- Ophthalmology review
- Renal function and estimated GFR measured
- Test for microalbuminuria (result was negative)
- Weight, height and BMI measured three times during the last 12 months
- BP recorded on two occasions during the past year
- Podiatrist visit six months ago
- Varenicline (Champix) initiation for smoking cessation three months ago
What additional aspect of care is required in order to bill Medicare for John’s first diabetes cycle of care?
Select an answer
The cycle of care minimum requirements are:
Every 6 months |
Measure weight, height, BMI
Measure BP
Examine feet |
Every 12 months |
Measure HBA1c
Test for micro-albuminuria
Check estimated GFR
Cholesterol and triglyceride test
Provision of self-care education
Medication review
Check SAP – smoking, nutrition, alcohol and physical activity |
Every 24 months |
Full eye check |
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 17: Fiona - Herpes simplex
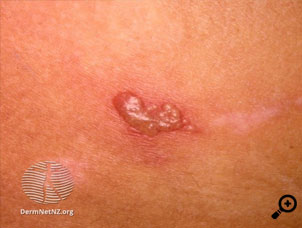
Fiona, aged 42 years, presents with back pain. As you are examining her lower lumbar and sacral area you notice scarring and blistering on her buttock (see picture).
When you comment on it she indicates that she has been getting them “on and off for years” and she doesn’t worry about them any more as they settle after a week or so.
What is the most likely diagnosis?
Select an answer
Herpes simplex can occur anywhere on the body. Once recurrent the vesicles tend to be smaller and more closely grouped. Occasionally white patches or scars may occur at the site of the recurrence.
Benign familial pemphigus is a rare disorder occurring in the third or fourth decade. It typically begins as a symmetrical, painful, erosive rash and is usually confined to the flexures.
Bullous impetigo and fixed drug eruptions are examples of other acute localised blistering conditions. Bullous impetigo is usually much larger blistering and often with the yellow crusting of impetigo.
There has been no history of recent medications to suggest a fixed drug reaction.
Cutaneous mastocytosis is usually a childhood illness. It is caused by a gene mutation that leads to clonal expansion of mast cells and itching, swelling and blistering of affected skin especially if rubbed or scratched. When it occurs in adults it is often itchy and is associated with systemic symptoms e.g. flushing, itching, low blood pressure etc.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 18: Patrick - Pulmonary embolism, treatment
Patrick, a 68-year-old farmer, had been well until his recent diagnosis of pancreatic cancer. He underwent biliary bypass surgery, and was discharged home to his farm to spend time with his family and consider whether he will choose to commence chemotherapy.
Today, he presents with sudden onset of severe shortness of breath. He has coughed up blood on his way to see you.
On examination his vital signs are: Temperature 36.4° C, P 130/minute and regular, BP 90/55 mmHg, respiratory rate 30/minute, 02 saturation 82% on his right arm.
Based on the most likely provisional diagnosis what is the most appropriate anticoagulant to commence?
Select an answer
The provisional diagnosis is acute pulmonary embolism (PE). The acute management of Patrick should include oxygen, analgesia and anticoagulation. Because he has evidence of haemodynamic compromise with a BP <90-100mmHg a parenteral anticoagulant is recommended e.g. enoxaparin or dalteparin and often as a twice daily routine especially in older patients, extremes of weight or with a malignancy. In addition there is currently insufficient evidence regarding efficacy of apixaban, rivaroxaban or dagibatran to recommend their use for patients with VTE and active cancer. Warfarin should never be commenced in isolation.
Oral anticoagulants (e.g. apixaban) are not first-line for VTE in pregnancy or for cancer-related VTE.
Unfractionated heparin IV is usually used for patients with severe kidney impairment or who have high risk of active bleeding and rapid reversability is required.
Fibrinolytic therapy may be of benefit in PE with haemodynamic compromise, however his recent cancer history may mitigate this as an option.
Patrick is in the high pre-test probability group for PE with age >65 years, recent surgery, active malignancy, tachycardia and haemoptysis. Pancreatic cancer is one of the cancers associated with a high risk of venous thrombosis (also brain and ovarian).
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 19: Mary - GORD
Mary, aged 58 years, has attended your practice regularly for the past 10 years. You have recently diagnosed her with hypertension, and a trial of lifestyle measures has not lowered her blood pressure significantly. You recommend pharmacological therapy.
Her medical history includes gastro-oesophageal reflux (GORD), for which she takes omeprazole 20 mg daily when necessary.
She has no known allergies.
In light of her history, which one of the following anti-hypertensive medications would you AVOID prescribing for Mary because it may aggravate her GORD symptoms?
Calcium channel blockers can reduce the tone of the lower oesophageal sphincter and impair oesophageal clearance, thereby facilitating gastro-oesophageal reflux. Symptom exacerbation has been shown to occur more with amlodipine and least commonly with diltiazem, with new symptom development most frequently with verapamil and least with diltiazem. The risk is higher with dihydropyridine CCBs than with non-dihydropyridine CCBs.
Other medications that may cause or contribute to GORD symptoms include:
- Aspirin and NSAIDs
- Benzodiazepines
- Bisphosphonates
- Anticholinergic drugs including tricyclic antidepressants
- Nitrates
- Theophylline
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 20: Mrs Klein - Burn first aid management
Mrs Klein races into the practice with her 5-year-old son Peter. He knocked the pot of boiling soup from the bench, which has burnt his left outer thigh.
Peter is crying and has a pack of frozen peas wrapped in a wet towel on the burn.
What is the most appropriate next step?
Select an answer
The application of cool to cold (around 15°C) running water to the burn for 20 minutes total duration is considered to be the gold standard for burns first aid.
This should be the first aid within three hours of a burn if it has not already occurred. This will reduce the likelihood of extension of the burn size and depth. It is important to avoid hypothermia especially in children, so first aid should be applied only to the burn area and the child should otherwise be kept warm.
Ice or ice slurries should be avoided as they can cause additional tissue damage. Hydrogel burn products are useful dressings but not as a first aid measure and should not be applied at this stage unless there is no access to water.
Analgesia according to the condition of the child should be provided but this should not be a topical application. Effective first aid can reduce the need for analgesia. Oral paracetamol or NSAIDs, stepping up to opioids, or even IV opioids may be required (fentanyl intranasal is a rapid option used in hospital settings).
Assessment of the depth and extent of the burn is an important step, once first aid is commenced. Sensation and capillary refill are important to assess the depth. The patient’s hand should be used to assess the extent of the burn. In a child the palmar aspect including fingers represents 1% total burn surface area. Children with >5% surface burn area require transfer, or if the face, hands, major joints, feet or genitals are involved.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 21: Leala - Acute asthma
Leala, aged 8 years, presents in the evening at the local emergency department with both her parents.
Leala saw her GP two days ago with an asthma flare-up associated with a viral respiratory tract infection, but her parents are now concerned that her asthma has worsened and is not settling with her regular reliever and preventer medications.
They gave her five puffs of salbutamol via an inhaler just before they came to the hospital.
On examination what is the most reliable parameter for assessing the severity of Leala’s acute asthma?
The most important and reliable parameters in assessment of asthma severity are:
- General appearance/mental state (agitated/or distress, confused/drowsy)
- Work of breathing – accessory muscle use and recession
Initial oxygen saturation in air, heart rate and ability to talk are helpful but less reliable. Oxygen saturation is purely a measure of oxygenation. It may be reduced in the absence of significant airway obstruction due to factors such as atelectasis and mucous plugging of airways. In addition it may be preserved in the presence of deteriorating ventilation (with CO2 retention).
A tachycardia can be a sign of severity but is also a side effect of beta agonists e.g. salbutamol.
Wheeze intensity, pulsus paradoxus and peak expiratory flow rates are not reliable.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 22: David - Cluster headache treatment
David, a 32-year-old man, presents because of recurring severe right-sided headaches.
These are located over the left eye and have been occurring 2-3 times a day for the past week. He is usually woken at about 6am every morning and this headache lasts about an hour. The other episodes last about 15-30 minutes.
He has had no associated nausea or neurological symptoms, but has noticed his left eye also gets red and tears and his nose feels stuffy. He had similar symptoms for a month last year and then they settled.
What is the most appropriate preventive treatment?
This is a classic story of cluster headache, which is one of the trigeminal autonomic cephalgias. These are distinct from trigeminal neuralgia because of presence of autonomic symptoms and generally no cutaneous trigger.
First line preventive treatments include verapamil, topiramate, sodium valproate, gabapentin and melatonin (in high doses). Verapamil has fewer side effects and is recommended as first drug to choose. Anecdotally immediate-release is more effective than the sustained release preparation.
Prednisolone or naratriptan (oral) is used as a bridging treatment to control the cluster headaches while the preventive drug reaches an effective dose.
Sumatriptin IV or intranasal, rizatriptan or zolmitriptan orally can be used for acute treatment. Oxygen 100% 15L/min by inhalation via a tight fitting non-rebreathing mask for 15-20 minutes can also be used for acute treatment.
Ibruprofen is a first line treatment non-opioid treatment for acute migraine and tension headache.
Amitriptyline is a preventive treatment for frequent or chronic unremitting tension-type headache.
References
- Therapeutic Guidelines. (2017). Neurology. Headache. Cluster headache. (eTG March 2021).
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 23: Salma - Periconception nutrition
Salma, a 26-year-old woman, attends the GP for removal of her Implanon® as she and her partner wish to start a family.
The GP undertakes a nutritional assessment and reinforces aspects of Salma’s diet. She also explains the need for nutritional supplements specifically the need to start folic acid supplementation now.
Which additional nutritional supplementation is most appropriate to commence?
The NHMRC recommends women should start a dietary supplementation of 150mcg of iodine prior to a planned pregnancy or as soon as possible after finding out they are pregnant. The NZ Ministry of Health recommends women should start dietary supplementation of iodine when planning a pregnancy (ideally for at least four weeks before conception and 12 weeks after conception).
Folic acid (400-500 µg), as identified, should be commenced at least four weeks prior to pregnancy and for the first 12 weeks of gestation.
Other nutritional supplements should be considered in specific circumstances:
- Vitamin D, in women identified by blood test as vitamin D deficient
- Iron, if identified as iron deficient by blood tests
- Vitamin B12 for all vegan and vegetarians (2.6 µg per day or IM injection 1000 µg/ampoule)
- Calcium, in women with inadequate dietary intake (<1000 mg daily)
Vitamin A from normal dietary sources does not pose a risk at normal levels, but if supplements are being used they should be limited to 3000 IU/day due to the increased risk of miscarriage and CNS malformations.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 24: Leon - Scrotal pain
Leon, a 58-year-old man, presents complaining of three days of left scrotal pain. It started on the last day of a one-week bicycle ride for Bike Week and the pain has gradually worsened. He has no urine frequency, painful urination or discharge.
On examination his temperature is 37.5°C, there is mild hemi-scrotal swelling and postero-lateral erythema, induration and tenderness on palpation. The upper pole of left testes is moderately tender. Gentle scrotal elevation relieves the pain.
What is the most likely diagnosis?
Select an answer
Epididymitis or epididymo-orchitis is one of the most common causes of scrotal pain in adults. While it can be an acute infection with acute scrotal pain and swelling with fever, rigors, and lower urinary tract symptoms, it usually has a more gradual course.
Pre-disposing factors include sexual activity, heavy physical exertion and prolonged periods of sitting (e.g. bicycle/motorbike riding). It is believed to be caused by retrograde passage of urine (reflux) from the prostatic urethra.
Signs considered to be strong predictors of epididymitis include pain isolated to the top of the testes, positive Prehn’s sign (pain relief with elevation of scrotum) and an intact cremasteric reflex.
In adults <35 years this is most likely due to Chlamydia trachomatis (50% of cases) or Neisseria gonorrhoea (usually associated with purulent discharge). In men over 35 years of age E. Coli is the more common pathogen.
Torsion of the testes is more likely to occur in children or adolescents (13-16 years) and usually presents with sudden onset of pain associated with nausea or vomiting.
Torsion of the testicular appendage usually has a more gradual onset over 1-2 days and has a peak incidence in pre-pubertal boys (peak 11 years of age). Tenderness is often in the upper pole of the testis and sometimes a ‘blue dot' sign can be seen (necrotic appendage seen through the skin).
A haematocoele is usually associated with trauma. Testicular cancer is usually painless but can present with mild pain in about 15% of cases.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 25: Joan - Hypertension management, diabetes
Joan is a 40-year-old woman who has had Type 2 diabetes for 10 years. She also has microalbuminuria, grade II retinopathy and mild chronic kidney disease. She is not currently on any antihypertensive medication.
She is reviewed by you today because her blood pressure has been elevated at the last two visits. Today her blood pressure is 145/98 mm Hg, and her home blood pressure measurements over the past two weeks also demonstrate a consistent elevation.
Which one of the following is the most appropriate initial medication to treat her hypertension?
Select an answer
The 2016 National Heart Foundation Guidelines advise that for patients with diabetes and hypertension, or for patients with chronic kidney disease (CKD) and hypertension, any of the first-line anti-hypertensive drugs are recommended. However, if the patient has CKD and hypertension and the presence of micro or macro-albuminuria, an angiotensin receptor blocker (ARB) or angiotensin converting enzyme (ACEI) inhibitor should be considered as first line therapy.
In this patient, perindopril, an ACEI would be first choice. Whilst irbesartan is an ARB it is combined with hydrochlorthiazide. It is generally recommended to commence anti-hypertensive therapy with a single agent, and later add a second agent if required. Starting with a combined agent may be considered in patients with a very high baseline BP, however the benefits and limitations of doing so need to be carefully considered. (2016 guidelines, page 43.)
Therapeutic Guidelines advises that ACEIs and ARBs are particularly important in slowing progression of kidney disease in patients with diabetes.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 26: Medico-legal social media
A doctor is on placement in a rural hospital and becomes aware of an adverse outcome for one of her patients.
She plans to post her experience online for self-reflection and to help others learn from the experience.
What is the most appropriate approach in managing confidentiality issues?
Select an answer
Doctors have an ethical and legal obligation to maintain patient confidentiality, and this applies to online posting in forums, blogs, and social networking sites in public and private forums. The most appropriate and effective way to maintain confidentiality is to have firstly received the patient’s consent and to acknowledge this on the post.
When posting it is important to remember that the patient should not be identifiable from the sum of the information online, not just based on a single post. Other postings on the same site are easily accessed and searched and could potentially provide additional information that could make the patient identifiable.
Using a pseudonym may not be adequate on its own to de-identify a patient, and changing case information and/or delaying the post are useful additional strategies.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 27: Sharon - Optic neuritis, MS
Sharon, aged 36 years, presents with two days of worsening vision in her right eye.
She tells you that her vision was initially a bit blurred, but now she can’t see much detail with that eye and colours appear a bit washed out. Since yesterday she has also had some dull aching pain behind the right eye, which seems worse with eye movement.
Sharon is generally well with no significant medical history and no previous eye problems besides myopia, which is treated with glasses.
On examination, her eyes are not inflamed and her visual acuity is right 6/18 and left 6/6 with her glasses on. There is red-green colour confusion with Ishihara testing in the right eye compared with the left and there is a relative afferent pupillary defect present. Fundoscopy with an undilated pupil appears normal.
What is the most important investigation to arrange?
Select an answer
The most likely diagnosis is optic neuritis, with classical history and examination findings.
Optic neuritis involves the acute inflammation of the optic nerve, and results in painful loss of vision. Two thirds of cases of acute optic neuritis are retrobulbar and fundoscopy is initially normal. The commonest cause of optic neuritis is idiopathic demyelinating optic neuritis, however, it is a symptom that can strongly suggest demyelination associated with multiple sclerosis (MS). 85% of people who develop MS start with a clinically isolated syndrome (CIS) or ‘first demyelinating event’, and of those 15-21% have optic neuritis as the CIS. Other conditions to consider include infection, diabetes, para-infection (such as sinus disease or encephalitis) or autoimmune disease (e.g. systemic lupus erythematosus, Sjogren syndrome, sarcoidosis).
An MRI is the most important baseline investigation to help predict the risk of developing clinically definite MS. This should be ordered in the context of early referral to an ophthalmologist for confirmation of the diagnosis and initiation of treatment as intravenous steroids speed recovery in acute demyelinating optic neuritis. (A diagnosis of MS requires lesions or symptoms to show dissemination in space and time.)
Lumbar puncture is now used less commonly for the diagnosis of multiple sclerosis, but can be useful in a patient with normal or atypical MRI.
Visual evoked potential is helpful if the diagnosis of optic neuritis is uncertain.
In typical cases blood tests are not useful but should be considered for atypical cases e.g. patients over 50 years of age, or in males. This could include a fasting glucose and antinuclear antibody investigation or chest xray (for suspected sarcoidosis).
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 28: Miranda - Postcoital bleeding
Miranda, a 33-year-old woman, presents to the GP because of vaginal bleeding post-intercourse. It occurred two nights ago and when her friend said that it could be serious she decided to get “it checked”. She had no pain and has not noticed any vaginal discharge apart from the small blood loss.
Miranda is on the combined oral contraceptive pill. Two months ago she became sexually active with her new male partner following a ‘split’ six months prior with her previous partner of four years.
Previous pap smears have been normal and she had a cervical screening test just last year which was normal. A speculum and pelvic examination are normal.
What is the most appropriate next management step?
Select an answer
The Royal Australian and New Zealand College of Obstetrics and Gynaecology (RANZCOG) flowchart for abnormal vaginal bleeding identifies consideration of the sexual history is an important first step, with appropriate testing as well as a co-test (HPV and LBC).
Miranda, however, has had a recent normal cervical screening test, but has had a partner change in the last 12 months. This is an indicator for testing for chlamydia. Thus an endocervical swab for NAAT (which is highly sensitive) is the most appropriate management step. A co-test could be performed with a chlamydia test requested added, however identifying the presence of chlamydia is the most important component in this scenario.
RANZCOG advise that a single episode of postcoital bleeding in a woman with a normal cervix appearance and normal cervical screening does not require immediate referral for a colposcopy. However colposcopy is mandatory for recurrent or persistent postcoital bleeding to exclude cervical cancer.
A pelvic ultrasound is recommended for persistent intermenstrual bleeding.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 29: Georgia - Chronic heart failure, exacerbation
Georgia aged 66 years, has a history of hypertension, chronic heart disease, hyperlipidaemia, irritable bowel, right knee arthritis.
She presents because she has put on 2.5 kg of weight over the last two days (she weighs herself daily) and has noticed mild ankle swelling. Further history and examination including ECG is unremarkable.
The most appropriate management at this presentation is:
This exacerbation does not require hospital admission at this stage. Her weight has increased by 2kgs over two days and the Guideline recommendations suggest review by a GP for a temporary increase in the dose of diuretics e.g. single multiple of the usual diuretic dose for three days.
Spironolactone may be an appropriate option if she has improved with the diuretic but needs added medication for heart failure control.
Also, while it is important to review her medications, this would occur after a positive response to the diuretic. This could involve increasing her enalapril.
Reduction of her beta blocker dose (carvedilol) could be considered if increasing congestion develops that is not managed with an increase in the diuretic dose.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 30: Julia - Diabetic ketoacidosis
Julia, a 15-year-old female, has spent the weekend at a friend’s beach house. Her friend’s parents have brought Julia into the regional emergency department because she has had nausea, vomiting and abdominal pain today and has become more drowsy.
On examination Julia seems pale, has rapid but regular deep breathing, weak pulse 110 beats/minute, blood pressure is 100/60 mmHg, and temperature 36.80 C. She has delayed central capillary refill.
Investigations reveal:
Arterial
|
Result |
Normal range |
pH |
7.1 |
7.35-7.45 |
PO2 |
104 |
80-100 mmHg |
PCO2 |
22 |
35-45 mmHg |
AHCO3 |
5 |
24-32 mmol/L |
Venous
|
Result |
Normal range |
Haemoglobin |
165 |
120-160 g/L |
Sodium |
126 |
137-143 mmol/L |
Potassium |
5.0 |
3.2-4.3 mmol/L |
Chloride |
92 |
98-108 mmol/L |
Bicarbonate |
6 |
22-23 mmol/L |
Glucose |
42 |
<8 mmol/L |
Acetoacetate |
3 |
<0.1 nmol/L |
Anion Gap |
33 |
7-17 mmol/L |
What is the most appropriate initial management?
Select an answer
The diagnosis in this scenario is diabetic ketoacidosis (DKA). The biochemical criteria for this diagnosis are:
- Serum glucose >11 mmol/L
- Venous pH <7.3 or bicarbonate < 15mmol/L
- Ketosis – either ketonaemia or ketonuria
The goals of management are to:
- Correct dehydration
- Reverse ketosis, correct acidosis and glucose
- Monitor for complications of DKA – cerebral oedema, hypo/hyperkalaemia, hypoglycaemia
- Identify and treat any precipitating cause – missed/reduced insulin dosing, infection
Julia has evidence of severe dehydration/shock (pale, tachycardia, hypotension, delayed central capillary refill) thus the most appropriate initial management would be resuscitation with 10ml/kg 0.9% sodium chloride bolus and reassessment.
Following this fluid replacement should be calculated and administered as 0.9% sodium chloride with added potassium (contraindicated if the patient is anuric or the potassium Is >5.5 mmol/L). While the potassium appears normal or even high (as in this case) there is a whole body potassium deficiency which requires replacement.
Insulin infusion begins after initial fluid resuscitation. This must be managed in a critical care area. Insulin is essential to turn of ketogenesis and reverse ketoacidosis. Insulin can be given subcutaneously (pH >7.2).
Sodium bicarbonate is not routinely recommended because it may cause a paradoxical CNS acidosis and the metabolic acidosis usually responds to adequate rehydration and insulin replacement.
0.9% sodium chloride with 5% glucose and potassium chloride (as required) can be used once the blood glucose level is ≤ 15mmol/L.
A more detailed description of management of DKA is provided in the references.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain