Introduction
Welcome to this multiple choice question (MCQ) activity. It is one of a series of activities designed to give you an opportunity to test your knowledge to help you to identify strengths and gaps, to provide you with answers and reference material for further review and over time give you the opportunity to reflect on your progress.
All Registrars, at all training levels, in GPTQ will be completing these. GPTQ will also review your answers compared to your peers and give you feedback.
In this activity the multiple choice questions are single best answer of five (5) options.
In addition there are two other rating questions for you to complete. They appear after you have chosen your answer to the MCQ.
Option weighting. The first series of questions asks you to weight each answer according to likelihood of being correct (in MCQs options are all possible but some are more likely/correct than others). You need to drag each option slider to identify your perception of the weighting for that option.
Question confidence rating. This rating relates to how confident you are about your answer to the question as a whole. You can click on the rating boxes or use the slider. Your confidence rating will be reviewed at the conclusion of the activity so you can reflect on how confident you were across each question and across the whole activity.
Version: March 2021 v1
Instructions
In this MCQ activity there are 30 MCQs for you to work through. You can work through them sequentially or choose questions from the menu in any order.
After you complete the MCQ, option rating and question confidence rating you are required to press the submit button to record your answers. Once you press the Submit button you will not be able to change your answers. You will immediately receive the correct answer and feedback so that you can compare them with your own answer. There will also be references provided for further reading.
At the end of the activity there is a conclusion screen that summarises the topic of each MCQ, whether your answer was correct/incorrect, your confidence level and the references for each MCQ. You can also print this summary screen so that you can explore the references at a later date.
Ideally you should complete this activity in one sitting, however you can click 'Save and close' to save and re-open it if you need to complete it in stages.
This activity should take 60 minutes to complete, or longer depending on whether you also explore the reference material at the same time.
Question 1: Sophia - Rubella
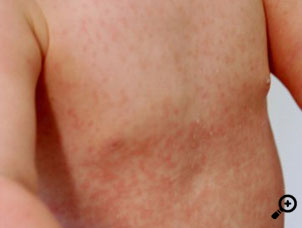
Sophia, 3 years old, presents with a generalised rash. Her mother says that Sophia has been unwell for 6 days with a runny nose, mild cough, and mild fevers. The rash started two days ago and has quickly spread to her neck, trunk, arms and legs.
Sophia has been well in the past. She and her siblings have never been immunised.
On examination her vital signs are normal apart from a temperature of 37.8°C. Her ears and throat are normal and she has mildly tender posterior auricular and posterior cervical lymph nodes.
The appearance of the rash is shown in the picture.
What is the most likely diagnosis?
Select an answer
The clinical scenario including the presence of tender posterior auricular and posterior cervical lymph nodes cervical lymph nodes and the distribution and appearance of the rash suggests the most likely diagnosis is rubella. However, a non-specific viral exanthema is also a differential diagnosis to consider.
Measles is uncommon in Australia and despite not being immunised it is unlikely unless there has been contact with someone who has returned from overseas with the virus. The absence of conjunctivitis also makes this diagnosis less likely. Children with measles may display Koplik spots in the mouth; a red blotchy rash usually starts on the face on the 3rd day of illness, and then spreads to trunk and then beyond.
Roseola infantum usually has a history of high fevers before the rash appears, and the rash mainly affects the trunk and rarely spreads to the arms, legs, neck and face.
The rash of erythema infectiosum (parvovirus B19) usually starts with a “slapped cheek” appearance (which is absent in this scenario) and is then followed a few days later by a pale pink reticular rash on the limbs and sometimes the trunk.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 2: Bob - COPD spirometry interpretation
Bob, aged 60, is a retired builder and a new patient. He presented yesterday because of chronic cough and gradually worsening breathlessness over the past few years. He is currently smoking about 5 cigarettes per day.
You arranged for a chest x-ray and spirometry. Bob couldn’t stay for the spirometry yesterday so returned today to complete the test.
The nurse brings in his spirometry results (shown below).
Test |
Predicted |
Pre bronchodilator |
% predicted |
Post bronchodilator |
% predicted |
FVC (L) |
4.83 |
4.75 |
98 |
4.73 |
98 |
FEV1 (L) |
3.76 |
1.79 |
48 |
1.85 |
49 |
FEV1/FVC (%) |
77 |
38 |
|
39 |
|
PEFR (L/min) |
576 |
403 |
69 |
415 |
72 |
Key: FVC Forced vital capacity; L litres; FEV1 Forced expiratory volume in one second; PEFR peak expiratory flow rate
What is the most likely diagnosis based on these results?
Select an answer
A low FEV1 pre bronchodilator indicates airflow limitation (also termed obstruction); typically, in chronic obstructive pulmonary disease (COPD) or asthma this will be less than 80% of the predicted value for age.
A restrictive lung disease pattern would generally result in a more reduced FVC; this can be accompanied by a normal or low FEV1.
The ratio of FEV1/FVC helps to distinguish between obstructive and restrictive lung disease. In patients with normal lung function this would be 0.8 or better. In obstructive lung disease (e.g. COPD or asthma) the FEV1/FVC would be less than 0.7; in restrictive lung disease (such as pulmonary fibrosis), the ratio would be normal or high.
Reversibility refers to any change in lung function after a bronchodilator has been administered – typically 15 minutes after 4 puffs of salbutamol. If there is an improvement in the FEV1 of 200mL and/or ≥12% when compared with pre bronchodilator FEV1 this is considered significant reversibility. Patients with asthma show significant reversibility on spirometry, and this is one of the key distinguishing features between asthma and COPD.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 3: Francine - SLE
Francine aged 30 years, presents feeling generally tired for the last two months. Her past medical history includes asthma in childhood. She denies any recent symptoms suggesting infection. A thorough systems review is unremarkable apart from occasional mouth ulcers and troublesome painful finger joints. She works in a busy accountancy firm. She is happily married and trying, so far unsuccessfully, to become pregnant.
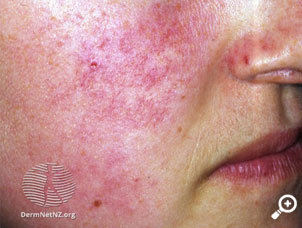
Her vital signs are: Temperature 37.5°C; BP 135/70; P 84 and regular; BMI 23; RR 12/minute. Her appearance is as shown in the image.
What is the most sensitive screening investigation?
Select an answer
Francine’s presentation suggests the diagnosis of systemic lupus erythematosus (SLE) (lethargy, arthritis, mouth ulcers, malar facial rash, a low-grade fever). Murtagh lists “polyarthritis + fatigue + skin lesions” as a diagnostic triad for SLE.
The ANA test is widely used as a serological marker of autoimmune disease. It is considered the best diagnostic test for SLE, as it is positive in virtually all patients with SLE. A raised test result however, is not specific for SLE, as it can also be raised in patients with rheumatoid arthritis, Sjogren’s syndrome, thyroid disease, chronic infectious diseases, systemic sclerosis, in patients on certain medications, and a low titre can be present in healthy people. So, by itself, it is not sufficient for diagnosis. However, the ANA test is considered the most sensitive test for confirming the diagnosis of SLE when accompanied by typical clinical findings. (BMJ Best Practice)
If ANA is positive, more specific tests are often performed based on clinical findings and ANA staining patterns.
In patients with a homogenous pattern ANA, antibodies against double-stranded DNA can be quantitated by the anti-dsDNA antibody test. Anti-dsDNA antibodies are highly specific for SLE (90%) and are often used to confirm the diagnosis, if present. However, the antibodies are only positive in approximately 60% of SLE patients. The level of this antibody may fluctuate with disease activity.
Antibodies directed against particular antigens within the cell nucleus are more strongly associated with particular rheumatic diseases. Testing for antibodies to these extractable nuclear antigens (ENA) is a useful follow-up test in patients with a positive speckled/peripheral ANA.
ESR and CRP are useful tests to monitor the disease activity, as they can be elevated in proportion to disease activity, but they are not diagnostic. They are non-specific markers and may be elevated due to an acute phase response from any cause.
This facial appearance is not classical of the melasma associated with pregnancy (the latter described as patchy brown, tan, or blue-grey facial skin discoloration of the central face, cheekbones and jawline). Whilst pregnancy may be important to check for (with HCG test) if Francine’s menstrual period is late, given she is lethargic and trying to become pregnant, the clinical presentation is more typical of SLE.
Rheumatoid factor is commonly found in SLE and has been associated with a more benign disease course. It is however not diagnostic.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 4: Clark - Severe acne
Clark, 17 years old, presents because he is embarrassed about his acne and wants something “to clear it up”.
In the past he has used topical benzoyl peroxide and adapalene but states that they didn’t make much difference. Most recently he has been using both topical treatments with oral doxycycline 100 mg. After 6 weeks of this combination treatment his acne hasn’t really improved. He confides that he is getting embarrassed to go out socially with his friends because of the acne and he really wants something that will work.
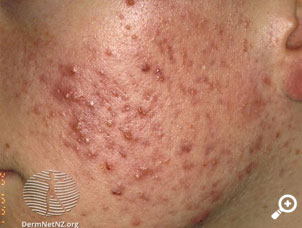
His facial acne is shown in the image.
What is the most appropriate next treatment option for Clark?
Select an answer
The clinical picture is of severe acne which is not responding to combination treatment and is having a negative social effect. Thus, most appropriate management would be a course of isotretinoin oral. (eTG)
While swapping to erythromycin oral could be considered, it is not the most appropriate option for Clark especially as he has all the indications for oral isotretinoin (severe acne, little improvement with combined treatment and a negative social effect).
Blue light treatment can improve acne and reduce inflammation however it is less likely to be as beneficial as isotretinoin oral.
Non-steroidal anti-inflammatory agents can be effective but only in some patients.
Topical clindamycin would not be expected to improve things if an oral antibiotic has not helped.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 5: Simon - Hypertension
Simon, aged 56 years, has attended for a ‘mole check’. He is an infrequent attender to the clinic because he is normally well and is on no medications. You take his blood pressure and it is 160/97mmHg. A reading at 5 minutes lying down in the nurse’s station is 150/90 mmHg and this is unchanged on a third reading at 15 minutes.
What is the next most appropriate management step regarding his blood pressure?
Select an answer
While the current recommendation for determining presence of hypertension is to take 3 BP measurements and then average the last two. The diagnosis should be based on multiple measurements taken on several separate occasions (i.e. at least twice, one or more weeks apart, or sooner if hypertension if blood pressure is severe). Out of clinic BP measurements are necessary for the diagnosis of white-coat and masked hypertension, which is estimated to occur in 10 – 20% of the general populations (eTG). If clinic BP is >140/90, or hypertension is suspected, ambulatory and/ or home monitoring should be offered to confirm the blood pressure level (Level I evidence). (2016 guidelines page 19). eTG also states that clinic BP measures are useful for screening but are inferior indicators of the patient’s actual BP.
Therefore, the most appropriate next step for Simon, whose BP has given significantly different measures over a period of 15 minutes, would be home BP monitoring or 24-hour ambulatory BP measures. The choice depends on indication, availability, ease, cost of use and patient preference. Home and ambulatory blood pressures are stronger predictors of cardiovascular events than clinic blood pressure measures.
With home BP monitoring it is important to recognize that the average morning reading is 10mmHg higher than the average evening one. Hence, if using home BP readings 50% need to be morning and 50% evening. In addition, you need to have at least 12-14 home BP readings for regression to the mean (i.e. if you take 30 readings you will get the same result as 12. However, four readings will give a different result). Thus, a week of home BP monitoring is required.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 6: Brenda - Sinus tachycardia
Brenda, a 27-year-old female, presents to the rural hospital having taken an overdose of risperidone of 30mg (5 times her usual dose) about 6 hours ago.
She was diagnosed with schizophrenia 6 years earlier and has been well controlled on medication.
Her overdose appears to relate to a recent job loss and a relationship breakup soon after.
What is the most likely finding on ECG?
Select an answer
Risperidone toxicity is most likely to result in a sinus tachycardia (50%), and in in a small number of cases can cause a prolonged QT interval. Torsades de pointes has not been reported as a result of the prolonged QT interval. Acute dystonias occur in 10% of cases and patients should be warned that these can occur up to 3 days after the overdose.
Tricyclic antidepressant overdose is more likely to result in broadening of the QRS complex, tachycardia, heart block block with the likelihood of significant broad complex dysrhythmias especially VT (if the QRS is > 160ms).
Benzodiazepine toxicity results in QRS widening (except for diazepam) and PR prolongation (except for oxazepam).
T wave inversion is the most reported ECG finding in lithium toxicity however heart blocks, PR prolongation and QT prolongation can occur.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 7: Vera - Thyroid nodule, investigation management
During a general examination of Vera, aged 42 years, a new patient to your general practice you find one non-tender nodule in her thyroid. It is firm and measures about 13 mm. She has previously been well, and there are no other significant examination findings.
The serum TSH is normal.
What is the most appropriate next step in investigating this nodule?
Select an answer
Thyroid ultrasound in the presence of a normal or high TSH is the investigation of choice to distinguish whether the nodule is cystic, solid/mixed, or part of a multi-nodular thyroid.
Thyroid scintography is appropriate in the presence of a low TSH to identify a hyper-functioning or hypo-functioning nodule.
A CT scan is not a routine component of investigation of the thyroid gland. If ever organised for other reasons it should be ‘non-contrast’ due to the risk of contrast induced hyperthyroidism or hypothyroidism in patients with nodular thyroid disease.
Serum free T4 concentration is the next appropriate investigation to consider in the presence of a normal TSH to rule out a central cause cause however it is not the most appropriate investigation in the presence of a thyroid nodule.
Ultrasound with fine needle biopsy would be the investigation of choice only if the patient was at risk of cancer, which includes:
- Palpable enlarged neck lymph nodes
- Rapid growth
- Symptoms of hoarseness, vocal cord paralysis or dysphagia
- Prior radiation
- Past history of partial thyroidectomy
- Family history of thyroid cancer or multiple endocrine neoplasia syndrome
- Past history of multiple endocrine neoplasia syndrome
A fine needle biopsy would also be considered depending on ultrasound features of the nodule (e.g. microcalcification, solid nodule >1cm).
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 8: Alan - GORD, Barretts’ oesophagitis
Alan, aged 61 years, presents with indigestion. He has now had three episodes of treatment with esomeprazole. The first time his symptoms settled after 3months; the second time he required 6 months of treatment and eighteen months ago, he started the medication again for a third time and has been on a low dose ever since. Despite the low dose he is now getting indigestion symptoms again.
Alan’s past medical history includes mild hypertension (being treated non-pharmacologically) and central obesity. He smokes 15 cigarettes / day. He drinks 6 stubbies of beer / weekend.
He has no significant family medical history.
Which factor places Alan at most risk of developing Barrett’s oesophagitis?
Select an answer
The major risk factors for Barrett’s oesophagitis (BO) are:
| Age |
relative risk rises 30% per decade after 40 years of age |
Male sex |
odds ratio 1.96 (95% CI 1.77 – 2.17) |
History of frequent GORD |
odds ratio 4.92 (94% CI 2.01 – 12.0) for long segment BO |
Abdominal central obesity |
odds ratio 2.24 (95% CI 1.08 – 4.65) for men |
Smoking |
odd ratio 1.42 (95% CI 1.15 – 1.76) |
Family history of oesophageal adenocarcinoma and/or Barrett’s oesophagitis |
relative risk 12-fold higher than GORD controls |
Alan has a number of these factors in combination which puts him at higher risk. In addition, he has symptoms despite being on PPIs.
Note: There is no evidence that alcohol consumption increases the risk of BO.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 9: Sara - Menorrhagia investigation
Sara, aged 46 years, presents because over the last 12 months her periods have been progressively getting heavier. She previously had regular 28-day cycles with bleeding for 5-7 days. However, they have now become heavier, more irregular (occurring every 19-35 days) and prolonged (lasting 8-10 days).
For the first 3-4 days she is changing her pads almost every two hours and in the last 5 months she has had two very embarrassing episodes of “flooding” while at work. She does have cramping pains but only when she passes large clots. There is no intermenstrual bleeding.
She has three children aged 20, 15 and 13 years old. She is divorced and not currently sexually active. Her cervical screening tests have been normal.
On examination Sara looks tired, but is otherwise unremarkable.
Results of last week’s full blood count, electrolytes, liver function tests and thyroid stimulating hormone, are normal.
What is the most appropriate next step?
Select an answer
Sara has heavy menstrual bleeding. It is important to try and identify the presence or absence of any underlying pathology, which will then determine subsequent treatment. The transvaginal ultrasound is a good initial investigation which will identify the presence of intrauterine pathology such as fibroids, adenomyosis, and polyps.
Risk of malignancy increases with age and an increased suspicion is warranted in a woman aged over 45 years of age. Medication should not be commenced until malignancy is excluded.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 10: Jeanie - Polymyalgia rheumatica investigation
Jeanie, aged 62 years, is a retired secretary who has no significant past history. She presents with a 3-week history of general malaise and stiffness. In the past month or so she has been tired, achy, and she has lost her appetite. She has noticed stiffness in her shoulders. She is finding it an effort to hang out her washing, and she also reports struggling to get out of her chair of an evening. When she wakes in the morning she feels stiff for about 3 hours. She doesn’t recall any recent fever or respiratory tract symptoms.
What is the most important initial diagnostic investigation to arrange?
Select an answer
The most likely diagnosis is polymyalgia rheumatica (PMR). It is characterised by proximal pain and stiffness of the shoulder and hip girdles with accompanying morning stiffness that lasts ≥1 hour. In most patients, symptoms first appear in the shoulder girdle.
C-reactive protein (and/or erythrocyte sedimentation rate, ESR) is the most important diagnostic investigation. Rheumatoid factor, ANA and TSH are all important to exclude other differential diagnoses. Temporal artery biopsy has a very low yield in patients with isolated PMR and is usually unnecessary unless there are symptoms of Giant Cell Arteritis (GCA) e.g jaw claudication (almost pathognomonic), severe headache, visual symptoms, scalp tenderness).
References
- Saad ER (2020). Polymyalgia rheumatica. Medscape
- Therapeutic Guidelines Pty Ltd. Rheumatology (2017) Polymyalgia rheumatic and giant cell arteritis. (eTG December 2020 edition).
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 11: Daisy - Chronic suppurative otitis media, ATSI
Daisy is a 3-year-old Aboriginal child brought in by her aunty who is concerned about ongoing discharge from both of her ears. She says that there has been yellowish fluid coming out of both ears intermittently for at least 2 months. She thinks that Daisy may have had a cold when the discharge first started. Upon further questioning, she reports that Daisy has also had a runny nose most of the time since then but is currently well with no fevers, no earache and good energy levels.
Nobody has noticed any problems with Daisy’s hearing, and there are no concerns about her development. Her aunty says that she hasn’t taken her to see a doctor before now as she didn’t seem unwell and she thought it would just clear up by itself.
Daisy has no significant past medical history, and no allergies.
On examination, Daisy is afebrile and well looking. The only clinical finding of note is purulent discharge in both of her auditory canals, and small perforations of both of her tympanic membranes. The tympanic membranes do not appear inflamed.
What is the most appropriate treatment?
Select an answer
All of these treatments are appropriate for treatment of ear conditions in Aboriginal and Torres Strait Islander children depending on the actual condition. In this case Daisy has chronic suppurative otitis media (CSOM), which is defined as persistent ear discharge through a persistent perforated tympanic membrane for at least 2 weeks.
Chronic suppurative otitis media |
Topical ciprofloxacin drops |
Acute otitis media without perforation |
Oral amoxicillin
Oral azithromycin stat if penicillin allergic or associated with trachoma infection in the eye |
Acute otitis media with perforation |
Oral amoxicillin and topical ciprofloxacin drops |
Otitis externa |
Topical ciprofloxacin drops OR
Topical framycetin/gramicidin/dexamethasone drops |
If discharge has been persistent for over 6 weeks and there are no features of acute infection as in Daisy’s case, topical antibiotics alone are recommended. Aminoglycoside drops are no longer advised due to the risk of ototoxicity especially in the presence of a perforated tympanic membrane.
Ear cleaning is very important, and regular mopping of the ear canal with dry tissue spears or syringing with povidone-iodine (Betadine®) is advised as an adjunct to any treatment.
The prevalence of CSOM is higher in Indigenous communities and can lead to hearing impairment and disability if not recognised or inadequately treated. Risk factors include passive smoking, childcare, use of dummies, bottle feeding (breastfeeding is protective) and social disadvantage.
Aminoglycoside drops are no longer advised due to the risk of ototoxicity especially in the presence of a perforated tympanic membrane.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 12: Emergency contraception - LNG
You are planning to deliver a session on contraception at the local high school. One of the areas you want to cover is emergency contraception.
Which one of the following statements is correct for the Levonorgestrel–Emergency Contraception (LNG-EC) method?
Select an answer
The most effective method for emergency contraception is the Copper intrauterine device (IUD) at 99%.
In Australia, the LNG-EC method of contraception (e.g. using Postinor-1 or -2) is indicated for use within 72 hours of unprotected sexual intercourse, however a recent update from the World Health Organisation, advises that it has proven effectiveness for up to 96 hours (4 days). Research suggests that it is 52–94% effective in preventing pregnancy, with its effectiveness improved the earlier it is given in relation to the unprotected coitus.
LNG-EC is available in Australia from pharmacies as over the counter medication, but a study as late as 2011 found 50% of Australian women were not aware that it was available without a prescription.
There is no risk of ectopic pregnancy with this method.
LNG-EC can be given as:
- Single stat dose of one 1.5 mg levonorgestrel tablet OR 2 x 0.75mg tablets; OR
- By divided dose, with one 0.75 mg levonorgestrel tablet stat followed by a second dose given 12 hours later.
Ulipristal acetate (UPA), a progesterone receptor modulator, as a 30mg single dose is 98% effective if taken within 72 hours of intercourse. Emergency contraception pills (ECP) with UPA are more effective between 72-120 hours after unprotected intercourse then other ECPs.
The Yuzpe method of emergency contraception is an alternative if women are unable to access LNG-EC. It involves the use of combined oral contraceptive pills. For this method, an anti-emetic is recommended to be taken with each dose.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 13: Dylan - Lacrimal duct obstruction
Dylan, a 3-month-old baby, is brought to you by his mother with a history of excessive tearing of the right eye since birth, as well as some yellow discharge from the same eye. His mother has tried antibiotic eye drops and massage at the corner of his eyes. She has also been washing his eye regularly with saline. On examination both Dylan’s eyes appear normal other than pooling of tears along the right lower eyelid.
What is the next most appropriate management of Dylan’s condition?
Select an answer
Watery, sticky eyes in young children is usually due to nasolacrimal duct obstruction. This occurs in about 5 % of infants, with 90% resolving by 12 months. While Dylan’s mother can be reassured that it is likely to resolve, the most appropriate management is the addition of regular warm compresses against the closed eye for 2-5 minutes 2-5 times a day. This is in addition to continuing nasolacrimal sac massage and keeping the eye clean with saline washes. Antibiotic eye drops can be used in short courses if infection develops – which would be indicated by an increase in amount and purulence of discharge, swelling, or redness of the eye.
The presence of any of the following red flags require immediate referral – photophobia, increase in size or unequal pupils, or a hazy/cloudy cornea suggestive of congenital glaucoma.
Treatment by nasolacrimal duct probing/surgery is only considered with tearing that persists after 12 months of age.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 14: Oliver - Prostate cancer
Oliver, a fit and active 62-year-old, has presented to discuss his treatment options following a diagnosis of prostate cancer by the urologist. He initially had a prostatic-specific antigen (PSA) test because his brother (aged 70 years) had been diagnosed with prostate cancer. His brother had significant side effects after his radical prostatectomy to treat the cancer. Oliver has heard that most treatments for prostate cancer commonly cause side effects.
The letter from the urologist indicates that he has localised cancer with one of four cores positive, clinical stage T2, a Gleason score of 6 and a PSA of 6.5 ng/ml.
While you plan to discuss a range of options, what is the most appropriate management to suggest to Oliver?
Select an answer
Oliver currently has low risk disease. The evidence suggests that mortality with his type of cancer is unchanged when managed with active surveillance compared with immediate aggressive interventions. Careful observation as an initial management strategy has been shown to be associated with the longest quality adjusted life expectancy.
Importantly active surveillance is not the same at “watchful waiting’ as it has a curative intent and involves more intense monitoring.
Active surveillance requires PSA testing every 3 months in the first two years after diagnosis then 6-monthly, with a physical examination including digital rectal examination. In addition, surveillance prostate biopsies should be offered within 6-12 months of diagnosis with repeat biopsies every 2-3 years thereafter.
Triggers for active curative intervention include:
- progression to a higher-grade tumour or higher volume tumour on surveillance biopsy
- PSA doubling in less than 3 years (progression further identified with repeat biopsy and multiparametric MRI in specialised centres)
- a change in patient preference towards definitive treatment
The main options for treatment of localised prostate cancer are active surveillance, brachytherapy, curative external beam radiation therapy, and radical prostatectomy.
Androgen deprivation therapy in combination with radiation therapy has been shown to increase survival in men with high and high/intermediate risk of occult metastases at initial presentation.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 15: Zahir - Iron deficiency, refugee
Zahir is a 28-year-old refugee from South Sudan who you are seeing today for discussion of results. You first saw her a week ago and ordered a number of investigations.
Zahir’s iron studies results are:
- Serum iron 10 ug/L (10-30/L)
- Total iron binding capacity 73 umol/L (45-70 umol/L)
- Transferrin saturation 11% (16-50%)
- Ferritin 20 ug/L (15-290 ug/L))
Relating to the commencement of iron therapy, what is the most appropriate management advice for Zahir?
Select an answer
Absorption of iron is enhanced by Vitamin C and inhibited by calcium containing products. In general, pure iron supplements (or those with added Vitamin C) are preferred over multivitamins as the amount of elemental iron contained in multivitamins is usually quite low and absorption can be reduced. Iron tablets should ideally be taken 1hr before or 2hr after food.
Iron levels should be checked again 3-4 weeks after starting oral therapy and monthly thereafter to evaluate the response. Therapy should be continued for 3 months after ferritin and haemoglobin levels normalise so that stores are replenished.
If oral iron is not tolerated, intravenous iron is the next preferred option. The haemoglobin should rise within 2-3 weeks in the majority of patients. The intramuscular route is not generally recommended as it is painful and causes permanent skin discolouration.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 16: CPR
You are planning to take your practice team and the visiting medical student through basic cardiopulmonary resuscitation (CPR).
Which of the following is correct regarding the Australian and New Zealand Committee on Resuscitation (ANZCOR) guidelines for basic CPR?
Select an answer
The ANZCOR guideline recommendations include:
- Compression-to-ventilation ratio be 30:2 for all ages.
- Chest compressions should be provided at a rate of approximately 100 – 120 /min.
- Rescuers must start CPR if the person is unresponsive and not breathing normally.
- All rescuers perform chest compressions for all who are not breathing normally.
- CPR commences with chest compressions
- Rescuers should aim to minimise interruptions to chest compressions.
- If the rescuer is trained and willing to include ventilations, then compressions must be paused to allow for ventilations
The initial steps of resuscitation are
DRS ABCD
Dangers
Responsiveness
Send for help
Airway
Breathing
CPR
Defibrillation
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 17: Rod - Obstructive sleep apnoea
Rod, aged 53, presents for renewal of his prescriptions. On general questioning, he says he has been feeling a bit tired and lacking in energy lately. He describes poor sleep and waking feeling unrefreshed.
What additional clinical information would most suggest the need for a sleep study?
Select an answer
The Epworth Sleepiness scale is a questionnaire about the likelihood of falling asleep in different scenarios, with a score of 9 indicating abnormal sleep possibly due to sleep apnoea.
There are a number of risk factors for obstructive sleep apnoea (OSA) which should prompt consideration of referral for a sleep study. These include:
- loud snoring especially that doesn’t resolve in lateral position,
- persistent daytime sleepiness,
- unstable medical conditions such as persistent hypertension, cardiovascular disease and
- use of medications that impair respiratory drive or cause upper airway dryness such as benzodiazepines and anticholinergics, including some antidepressants. (Citalopram has a relatively low anticholinergic effect)
Recurrent tonsillitis is not in itself a risk factor for sleep apnoea, although persistently enlarged “kissing” tonsils would increase likelihood.
A persistent erythrocytosis seen on blood tests may indicate sleep apnoea but is not the most suggestive factor for a sleep study.
Clinical examination of a patient with suspected OSA should include:
- body mass index (BMI especially if >35 mm/kg2) and neck circumference (>40cm) - as a high level of either of these increases risk of OSA
- assessment of upper airway patency using the Mallampatti scale (scores C and D are associated with an increased risk of sleep apnoea)
- state of dentition and palate
- blood pressure
- nasal patency
- checking for sinus disease
- a medication review
Spirometry is not routinely used to assess risk of sleep apnoea.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 18: Ash - Systemic juvenile idiopathic arthritis
Ash, aged 11 years, presents with his mother because of fatigue, persistent fevers and generalised muscle and joint aches and pains. His symptoms began about a month ago and his mother (a nurse) thought they would settle. He has however now missed several days of school.
She says that Ash has been spiking a fever late afternoon on most days, which settles completely by the evening. She adds that during the fever he often develops a pink rash on his torso and limbs which settles within an hour or two.
On examination Ash looks unwell but he is afebrile and his other vital signs are normal. He has generalised muscle tenderness on palpation and evidence of swelling and pain in the left knee and left wrist. He has a mild hepatomegaly but no splenomegaly. Examination is otherwise unremarkable.
What is the most likely diagnosis?
Select an answer
While the diagnosis of juvenile idiopathic arthritis (JIA) requires the presence of symptoms for least 6 weeks, there are a number of classic features in Ash’s presentation that make JIA the most likely diagnosis:
- The presence and regular pattern of spiking fevers, typically occurring once or twice a day;
- The presence of a transient, often linear, salmon pink macular rash on the trunk or extremities which appears with the fever and lasts only a short time;
- Generalised muscle aches and arthralgia; and
- Arthritis in one or more joints, which can occur with onset of fever and rash but can also appear months later.
Lymphadenopathy, especially axillary lymph nodes, may be present, as can pericarditis and pleuritis. Hepatosplenomegaly is often present.
Kawasaki disease is a differential diagnosis for systemic JIA, however this condition occurs in a younger age group (less than 5 years old) and does not have the classical pattern of fever that is seen in systemic JIA.
Acute lymphocytic leukaemia can present with joint pain and arthritis but often presents with severe pain in the metaphyses which awakens a child from sleep. It is a disease most likely to be misdiagnosed as JIA.
Postinfectious arthritis usually affects large joints and may often be indistinguishable from the early phase of JIA.
Acute rheumatic fever usually results in severe joint pain and the arthritis is usually migratory, not additive and associated with fevers.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 19: Brian - Laceration, suture removal
Brian is a 58-year-old fisherman. You have just excised a small lesion (possible BCC) from the dorsum of his hand and sutured the site.
When would be the most appropriate time for him to return for suture removal?
On the dorsum of the hand sutures are best removed between 10-14 days.
Location |
Timing |
Face |
3 – 5 days |
Scalp |
7 – 10 days |
Arms |
7 – 10 days |
Trunk |
10 – 14 days |
Legs |
10 – 14 days |
Dorsum hands or feet |
10 – 14 days |
Palms or soles |
14 – 21 days |
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 20: Sally - Heart failure, hypotension
Sally aged 67 years has a history of hypertension, hypercholesterolaemia, gastro-oesophageal reflux disease (GORD), ischaemic heart disease and chronic heart failure. Her medications include: perindopril, metoprolol controlled release, frusemide, and esomeprazole.
She comes to see you because she has had a few episodes of being light headed in the last few days and has fainted once. On further questioning these seem to occur with posture changes. On examination her pulse is 85 and regular, and her BP is 110/80 mmHgsitting and on standing for 2 minutes is 90/ 60 mmHg. Her cardio-respiratory examination is otherwise unremarkable and her electrocardiogram (ECG) is unchanged from previously.
The most appropriate next management step is to:
Select an answer
This patient has hypotension, which can be caused by a number of medications. In this situation reducing the frusemide first can be beneficial as the other heart failure medications have specific long-term survival benefits at maximal doses, whereas the diuretic is for symptom management.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 21: Anne - Elevated bilirubin – Gilbert syndrome
You are asked to review the pathology results of a patient, Anne, aged 32 years. Anne saw one of your colleagues last week complaining of general malaise. She works as a waitress in a restaurant, and 2 weeks ago was given a course of roxithromycin for a respiratory tract infection. Her general health is usually good although she is significantly overweight (body mass index 29). She is on the combined oral contraceptive pill (COCP).
Her full blood count is normal, as are her electrolytes. Her liver function test (LFT) results show:
Albumin |
40 g/L (34–48) |
Protein |
72 g/L (65–85) |
Total bilirubin |
34 μmol/L (2–24) |
Gamma-glutamyl transferase (GGT) |
30 U/L (<60) |
Alkaline phosphatase (ALP) |
80 U/L (30–110) |
Alanine transaminase (ALT) |
34 U/L (<55) |
Aspartate transaminase (AST) |
24 U/L (<45) |
What is the most likely explanation for Anne’s LFT results?
Select an answer
Anne’s liver function tests are normal apart from a raised bilirubin.
Unconjugated hyperbilirubinaemia in adults where other liver function tests are normal, is usually due to Gilbert syndrome or to haemolysis. Anne’s full blood count is normal.
Gilbert syndrome is a relatively common inherited condition affecting 3% to 5% of the population. It is due to impairment in bilirubin conjugating ability and is considered a benign condition. Test results show a persistent isolated increase in bilirubin. Gilbert Syndrome is usually identified by the finding of a mild elevation of bilirubin in a request for liver function tests ordered for another purpose. The bilirubin level is usually in the mildly elevated range, up to 40 umol/L, although normal values may occur, and results as high as 80 umol/L may be seen in patients who have not consumed food for several days or during acute illness. Further investigation is not considered necessary if other LFTs are normal.
Acute viral hepatitis would give a picture of hepatocellular damage with marked increases of ALT (three times greater than ALP) and AST, as well as bilirubin increases. A cholestatic picture would include a raised bilirubin and a raised ALP more than three times the ALT. Drugs such as roxithromycin, erythromycin and oestrogen give a cholestatic picture.
Typical LFT findings in non-alcoholic fatty liver disease (NAFLD) are raised ALT and AST, with a preserved ALT: AST ratio of 1.5, raised GGT and, occasionally, raised ALP. These findings commonly occur in the setting of features of the metabolic syndrome.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 22: Gayle - Multiple sclerosis treatment
Gayle, aged 36 years, has come to see you to discuss a diagnosis of relapsing-remitting multiple sclerosis (RRMS) after a recent visit to a neurologist. She had optic neuritis diagnosed 2 months ago, and investigations following this included an MRI which showed 4 brain lesions suggestive of MS. On review of her history you also note that she had an episode of trigeminal neuralgia 5 years ago.
The specialist indicated that he wanted to start Gayle on a highly effective treatment early. Gayle and her family are shocked and upset by the diagnosis, and Gayle wants to discuss treatment and side effects with you as she felt a little overwhelmed with the specialist.
What is the most appropriate initial treatment for Gayle’s MS to reduce the frequency of attacks and the rate of disease progression?
Historically the approach has been to start with the safest drugs, however increasingly the approach is to commence highly effective treatment early so the patient achieves a target called NEDA (no evidence of disease activity)—with NEDA, the patient is stable clinically, and has no relapses and no new lesions on magnetic resonance imaging. Thus a monoclonal antibody agent has the highest efficacy e.g.IV natalizumab or alemtuzumab.
Drug |
Efficacy |
Serious adverse effects |
|
Relapses (ARR,RRR) |
Disability |
New lesions on MRI (RRR) |
|
Alemtuzumab |
67% |
52% |
94% |
Thyroid autoimmunity
ITP
Haemolytic anaemia
Anti-GBM kidney disease (rare) |
Natalizumab |
68% |
54% |
92% |
Progressive multifocal leukoencephalopathy (rare) |
Azathioprine (an immunosuppressant) does have benefits similar to immunomodulators in patients resistant to or not eligible for immunomodulators.
Amantadine is effective short term for managing the fatigue in MS.
Oral prednisolone is used for moderate relapses with disability and unpleasant or worsening symptoms, and IV methylprednisolone for severe relapses (e.g. severe visual loss, paraplegia or brainstem symptoms).
Table reproduced from ETG. Available immunotherapies for MS.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 23: Margie - Lactation complications
Margie, aged 33 years, is one of your regular patients. She is very excited to be pregnant. She is also very keen to breast feed her baby after delivery, and you discuss this in detail at her 36-week visit. An examination of her breasts is unremarkable.
When considering Margie’s suitability for breastfeeding, what further clinical information or examination would indicate that breastfeeding is contraindicated?
Select an answer
HIV infection can be vertically transferred (from mother to infant) via breastmilk so for HIV infected mothers, breast milk alternative is advised where it is safe and available.
Breastfeeding has multiple benefits for the infant and mother and should be encouraged and promoted at every opportunity. There are few true contraindications to breastfeeding, and concerns and hesitations from mothers should be gently explored.
A history of HSV1 infection on the nipples is not a contraindication to breastfeeding unless there are active lesions; once lesions are resolved breastfeeding can resume.
Women of all weights can breastfeed, and the importance of good nutrition should be emphasised.
Inverted nipples can make breastfeeding more challenging, but most women will still be able to breastfeed successfully.
The effects of breast augmentation / breast implants on breastfeeding will depend on the reason for the surgery and the surgical procedure used. Breast implants are not a contraindication to breast feeding. Whilst they may be associated with insufficient lactation, breast feeding may be successful and women should be encouraged to breast feed.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 24: Sarah - Pregnancy, prescribing
Sarah, aged 29 years, is 15 weeks into her first pregnancy. You see from her notes that she is being managed by your local hospital maternity clinic and has presented today as she has a bad head cold. She tells you that she has been taking paracetamol but it hasn’t been helping much, and she wants to know what else she can take.
Prior to pregnancy she used to use fluticasone furoate (Avamys®) nasal spray with good effect whenever she got a bad head cold, and she is wondering if it is safe to use this.
After looking up your pregnancy database, you explain to Sarah that fluticasone furoate is a Category B3 drug – it has been taken by a limited number of pregnant women without any observed increase in frequency of adverse foetal effects, although studies in animals have shown an increased occurrence of foetal damage.
What is the most appropriate response to give to Sarah?
Select an answer
The Australian Government TGA established a classification system to assist practitioners prescribing drugs in pregnancy to assess the safety of these and counsel patients accordingly.
Apart from the category it is important to take into account other information when counselling the patient:
- The exposure to the foetus may be affected by
- Dose
- Route of administration
- Dosing regimen
- The timing of the exposure in the pregnancy e.g. the embryonic period (4-14 weeks amenorrhoea) is the time when exposure to potentially harmful drugs can cause structural birth defects
Furthermore, the Australian categorisation system is not hierarchical.
- Human data is lacking or inadequate for drugs in Category B1, B2, B3
- The sub-categorisation of the B category is based on animal data
- Allocation of a Category B status does not imply greater safety than Category C
These drug categories do not apply to breastfeeding, and safety of drugs during lactation should be considered separately to pregnancy.
Counselling should be non-directive and information given so that the patient can make a decision based on as much evidence–based data as possible.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 25: Jack - Pertussis vaccination
Jack, aged 7 years, is brought in to see you by his mother Natalie and his grandmother Shirley. Natalie is concerned because a child in Jack’s class at school has been recently diagnosed with whooping cough. On questioning, Natalie says that Jack has been well with no cough or fevers.
Natalie is also worried as she is 25 weeks pregnant. She tells you that she had a pertussis vaccination during her pregnancy with Jack, and has been recently well with no cough. Shirley also asks you about her risk of whooping cough as she will be helping out with caring for the baby after its arrival, and recalls being vaccinated about 12 years ago. Jack is up to date with his vaccinations.
What is the most appropriate management advice at this consultation?
Select an answer
All adults such as Shirley who will be involved in caring for young infants should receive a pertussis booster vaccination if more than 10 years have elapsed since their last vaccination.
The diagnostic test of choice for pertussis is a nasopharyngeal aspirate or swab (throat swabs are less sensitive), however Jack has no symptoms at this stage and probably does not need investigation.
Previous vaccination reduces the risk of pertussis, but infection is still possible in immunised individuals. Natalie should receive a pertussis booster in the 3rd trimester of each pregnancy, ideally from 20 weeks.
Antibiotic prophylaxis is recommended in households and childcare centres where there are susceptible infants and young children but there is limited evidence to support prophylaxis in schools or tertiary institutions unless there are two or more cases in the same room within a single incubation period. Jack is fully vaccinated, does not have symptoms and so is not likely to need prophylaxis.
Pertussis is a respiratory illness caused by Bordetella pertussis that can occur in any age group, but is most dangerous to young infants, patients who are elderly, immunocompromised or have chronic disease, and pregnant women. It is extremely infectious, and symptoms can vary from a mild upper respiratory type illness to life-threatening complications such as pneumonia and hypoxia.
Pregnant women are particularly vulnerable to complications in the later stages of pregnancy; antibiotic prophylaxis is recommended in women in the last month of their pregnancy if they have had close contact with a confirmed case of pertussis.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 26: Trina - Melanoma
Trina, aged 49 years, presents with a skin lesion on her left upper arm that she is concerned may be a melanoma. Her mother has had two melanomas removed over the past 15 years. Trina thinks that her mole has changed in shape and has darker spots in it.
Trina is otherwise well and on no medications.
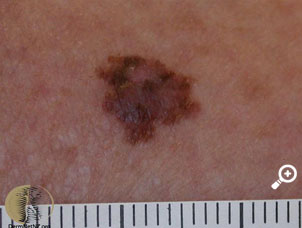
On examination the appearance of the lesion is shown in the image. There are no palpable axillary lymph nodes.
What is the most appropriate initial management?
Select an answer
The history of change to the naevus, the family history and the appearance of the lesion according to the ABCDEs of melanoma suggest a superficial spreading melanoma. Dermatoscopy may help confirm this further.
It is recommended that excision biopsy with a 2 mm margin (and as deep as subcutaneous fat) is the initial treatment of choice, even where there is confidence in the diagnosis. The excision biopsy allows for confirmation of the diagnosis and rational planning of the definitive treatment regarding the requirement for wide excision margins and the possible need for sentinel node sampling.
Wide excision margins are based on Breslow thickness - a margin of 1cm is recommended for melanomas < 1.0 mm thick.
Moh's surgery is a precise surgical procedure which involves carefully examining marked excised tissue under the microscope, layer by layer, to ensure complete excision. It is generally considered inappropriate for definitive treatment of a melanoma.
Punch, incision and shave biopsies are not recommended as they are frequently unsatisfactory and may result in misdiagnosis due to unrepresentative sampling.
Watchful waiting is inappropriate given the changes clinically according to the ABCDEs of melanoma.
A – Asymmetry
B – Border irregularity
C – Colour variation
D – Diameter over 6 mm (increasing diameter more important than size)
E – Evolving (enlarging, changing)
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 27: Maria - AF, warfarin bleed
You are a rural GP working in a local, regional hospital and are reviewing Maria, aged 82 years, on the ward. She had presented to the hospital following a large gastrointestinal bleed for which she required 3 units of packed cells.
Maria’s past history includes longstanding persistent atrial fibrillation, a right sided stroke 3 years ago and hypertension. Her medication on admission to hospital was warfarin (which was promptly ceased), metoprolol and enalapril.
Maria is worried about her risks of another stroke now she is not taking warfarin, but doesn’t want another bleeding episode.
What is the most appropriate long-term management option for Maria?
Select an answer
This patient’s CHA2DS2-VASc score is 6 (9.7% adjusted stroke rate per year). Her HASBLED score is 4 (8.7 bleeds per 100 patient years).
The most important management issue here is the reduction of her risk of stroke. The majority of embolic stroke in non-valvular atrial fibrillation is left atrial appendage thrombi. The most appropriate option, as a suitable alternative to long term anticoagulation, is left atrial appendage occlusion. Ablation of AF focal triggers is also an option for consideration in symptomatic paroxysmal or persistent atrial fibrillation.
Changing to rivaroxaban or dabigatran is not indicated as studies have indicated that they have a greater risk of GI bleeding than warfarin. This increased risk has not been shown with Apixaban, which may be an option, but as this was a large bleed it would still be safer to pursue a management pathway that obviates the need for anticoagulation.
Amiodarone or sotalol may control the rhythm but this does not impact on her stroke risk.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 28: Louise - Vulvovaginitis, prepubertal
Louise, an 8-year-old girl, presents with her mother. Louise has a white vaginal discharge and vulval redness and mild itch for the last two days. It has not settled with a dilute vinegar bath. Her mother is concerned that it is getting worse. Louise is now complaining of burning when she passes urine. Louise has no past history of any skin rashes, and has no allergies.
On examination there is moderate vulval redness, some linear scratches, an intact hymen and some white discharge. You take an introital swab.
What is the most appropriate treatment of Louise’s symptoms, if an infective cause is suspected?
Vulvovaginitis in prepubertal girls is usually due to dermatitis or psoriasis, and an infective cause is less common. If infective vulvovaginitis is diagnosed, the most common cause is Streptococcus pyogenes (Group A streptococcus). Other organisms may also be present (Haemophilus, Gardnerella), hence the value of an introital (not vaginal) swab.
The recommended treatment is cephalexin orally, if Group A streptococcus is isolated on a low vaginal swab; therapy is not guided by swab sensitivity results. While Streptococcus pyogenesis is susceptible to penicillins, perineal infections treated with penicillin tend to recur at a high rate.
Clindamycin or trimethoprim plus sulfamethoxazole can be used if there is an immediate hypersensitivity to penicillins.
Candidal vulvovaginitis does not occur in prepubertal girls and so clotrimazole or fluconazole are not appropriate.
Threadworms need to be considered, however there is likely to be a history of intense itch in the anal region (which can extend to the vulval region in girls). The itch is often worse at night or early morning when threadworm can be seen at the anus.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 29: Brenda - Childhood asthma treatment
Brenda attends with her 4-year-old daughter Sophie. She has come for a cervical cancer screening test but also asks you for a repeat prescription of salbutamol for Sophie. You ask about Sophie’s asthma and Brenda tells you that Sophie has flare ups of her asthma every 2-3 weeks, but that these are managed with salbutamol aerosol, 2 puffs every 4 hours as necessary. She is not on any other medications. In between the flare-ups Sophie has no symptoms. Brenda confirms that she is using a spacer to administer the salbutamol, and her demonstration of the technique is appropriate.
Sophie’s physical examination is normal.
What is the most appropriate management option for Sophie?
Select an answer
Brenda is describing a pattern of frequent intermittent asthma and preventer treatment should be considered given the frequency is less than monthly. The Asthma Management Handbook recommends a treatment trial of adding inhaled corticosteroids over montelukast oral 4mg once daily unless there are specific indications. Review in 2-4 weeks. (N.B. it is important to advise parents about the potential adverse psychiatric effects of montelukast.)
Low dose inhaled corticosteroid/long -acting beta 2 agonist combinations are not recommended for children 5 years and under, unless on the advice of a paediatrician.
Swapping to a long acting beta agonist (LABA) such as formoterol is not recommended as the part of the stepped approach to management.
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain
Question 30: Rowan - Concussion red flags
You are a general practitioner and have gone to watch your 15-year-old son, Rowan, play AFL football. During the game Rowan takes a high mark but comes down hard onto the ground and hits his head. He is slow to get up but takes the kick. Afterwards he seems a bit unsteady and his coach takes him off the ground. You go over to check on Rowan.
What clinical symptom or sign would suggest that Rowan needs urgent medical assessment?
Select an answer
All of these symptoms and signs suggest the presence of concussion. However, in the setting of an episode of concussion, neck pain is a red flag that requires urgent medical assessment.
Other red flags include:
- Increasing confusion or irritability
- Repeated vomiting
- Seizure or convulsion
- Weakness or tingling/burning in the arms or legs
- Deteriorating conscious state
- Severe or increasing headache
- Unusual behaviour change
- Double vision
References
Rate your overall level of certainty in answering this question.
Please select:
0. No idea / guess
1. Very uncertain
2. Uncertain
3. Certain
4. Very certain